If you’ve been searching for TMS Therapy, you may be looking for a proven solution to depression and other mental health conditions that haven’t improved with traditional treatments. At HWS Center, our board-certified TMS providers offer Transcranial Magnetic Stimulation (TMS), a safe, non-invasive treatment option that targets specific brain regions without systemic side effects.
This outpatient procedure keeps you fully awake during each TMS session, allowing you to return to normal routines right away. For patients who have not achieved relief with antidepressant medications or talk therapy, TMS has become an effective treatment backed by strong research and clinical trials.
TMS Therapy Near Me is an FDA-cleared, non-invasive procedure used to treat major depressive disorder, treatment-resistant depression, and other mood disorders. It offers renewed hope to individuals living with severe depression who have not responded to medication or psychotherapy.
Using an advanced TMS machine, a small electromagnetic coil is placed over the scalp to deliver controlled magnetic fields to specific areas of the brain responsible for mood regulation. This painless brain stimulation activates underactive nerve cells, restoring healthy brain activity and brain function.
Unlike medications, this drug-free treatment plan does not cause weight gain, fatigue, or memory loss. With a strong success rate and results proven in clinical trials, TMS is recognized as one of the best TMS therapy options available today.


TMS therapy continues to grow in popularity, especially for patients who need an effective treatment without the side effects of medications. Clinical trials and decades of research highlight its success rate for managing major depression, anxiety disorders, bipolar disorder, and post-traumatic stress disorder.
Many patients report enhanced mood, better sleep, increased energy, and improved focus after completing their treatment plan. TMS is helping individuals find relief and reclaim their daily activities with minimal disruption.
Get help with depression today! It’s important to know that you are not alone.
Searching for a “TMS clinic near me” means you may be struggling with more than just depression. TMS is widely used for major depression and treatment-resistant depression, but studies also show benefits for:
Anxiety disorders
Obsessive-compulsive disorder
Post-traumatic stress disorder (PTSD) and traumatic stress disorder
Bipolar disorder
Neurological conditions such as Parkinson’s, Alzheimer’s, and chronic pain
By targeting specific areas of the brain, TMS improves mood regulation, concentration, and emotional balance. Patients often notice positive changes in energy, sleep, and focus during their weeks of treatment.










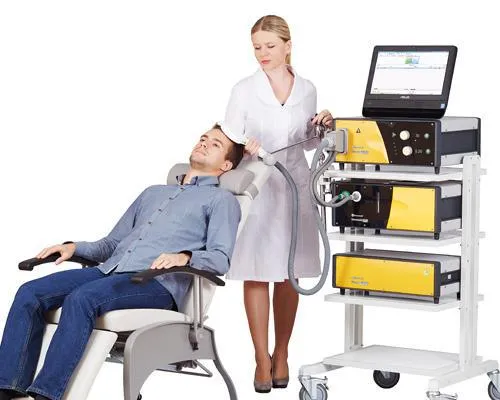
During a typical TMS session, a trained healthcare provider or nurse practitioner positions the electromagnetic coil on the scalp. The device delivers magnetic pulses that stimulate underactive brain cells in the prefrontal cortex, the part of the brain linked to mood and emotional stability.
Unlike whole-brain stimulation, TMS precisely targets only the area beneath the coil, improving depression symptoms by restoring healthy brain activity. Treatment usually involves five sessions per week over four to six weeks. Many new patients notice positive changes in mood and energy within the first 3–5 weeks.
TMS is considered safe, with minimal side-effects of TMS. The most common side effects include a mild tapping sensation, scalp discomfort, or slight headaches during initial sessions. These usually fade as treatment continues.
Unlike medication or electroconvulsive therapy, TMS does not cause weight gain, memory loss, or systemic side effects. Because it is an outpatient procedure, patients can resume daily activities immediately after treatment.
TMS may not be suitable for those with certain implants, a history of seizures, or metal near the head. Always consult a qualified healthcare provider before beginning any new depression treatment.
If you’re in Fort Lee, Englewood, North Bergen, or New York and have been searching for a “TMS therapy near me,” the HWS Center is here to help.
As a trusted TMS provider, we design a personalized treatment plan to address your unique mental health issues. Our board-certified clinicians accept most insurance providers, making insurance coverage simple for new patients.
Schedule your free consultation today and learn how the benefits of TMS therapy can support long-term mental wellness and overall well-being.
Unlike traditional treatments such as antidepressant medications or talk therapy, TMS is a non-invasive treatment that uses a TMS machine to deliver safe magnetic fields directly to specific areas of the brain involved in mood regulation. This targeted approach avoids systemic side effects while offering a strong user experience with a proven success rate for patients with resistant depression. This targeted approach ensures patients receive TMS right, avoiding systemic side effects while offering a strong user experience with a proven success rate for patients with resistant depression.
Research and clinical trials confirm that TMS is an effective treatment for both major depression and treatment-resistant depression. Patients often report reduced symptoms of depression, better sleep, and increased focus after just a few weeks of treatment.
Yes. Beyond major depressive disorder, TMS has demonstrated positive results for anxiety disorders, obsessive-compulsive disorder, post-traumatic stress disorder (PTSD), and even traumatic stress disorder. Studies continue to explore its benefits for neurological conditions such as Parkinson’s and Alzheimer’s.
Each outpatient procedure takes about 19 minutes. A trained nurse practitioner or healthcare provider places an electromagnetic coil on your scalp to deliver pulses that stimulate underactive nerve cells. You’ll remain awake, alert, and able to return to your daily routine immediately. This precision helps ensure TMS is done right, targeting only the specific areas of the brain involved in mood regulation.
TMS is well tolerated by most patients. Common side effects include mild scalp tingling or light headaches during the first few sessions. Unlike medications, TMS does not cause fatigue, weight gain, or memory loss, making it a safer alternative for those who did not improve with medication management.
Yes. TMS is FDA-cleared and performed by board-certified providers. It is considered safe for new patients who do not have metal implants in or near the head, seizure disorders, or certain neurological conditions. Before treatment, we coordinate with your primary care team to ensure TMS is the best fit for your needs. Our staff helps patients navigate Patient Portals to make the process as smooth as possible.
Many of our treatment programs are covered by insurance. Contact your insurance provider to verify benefits for mental health care.
We currently accept the following insurance plans:
Other insurance plans are in progress.
Self-pay plans would be discussed on an individual basis.
A standard TMS treatment plan involves daily sessions, five days per week, for about four to six weeks. Each therapy session lasts approximately 19 minutes. Many patients begin noticing improvements in mood and cognitive clarity within the first 2–3 weeks. Long-term success depends on the severity of symptoms and the patient’s unique needs. Follow-up sessions or maintenance treatments may be recommended to sustain the results. The treatment center staff will tailor a plan to ensure optimal, lasting outcomes based on your progress.
TMS therapy near me differs from antidepressant medications in both mechanism and side effect profile. While medications affect the entire body and often cause systemic side effects such as weight gain, fatigue, and gastrointestinal issues, TMS uses localized magnetic stimulation on targeted brain cells. This non-invasive treatment doesn’t circulate through the bloodstream and avoids many complications tied to long-term medication use. It is ideal for individuals seeking effective treatment without the burden of daily pills or systemic impact.
Yes. Numerous clinical trials and studies have confirmed the effectiveness of TMS in treating depression and other mood disorders. It has been cleared by the U.S. Food and Drug Administration and is endorsed by mental health care professionals worldwide. Ongoing research is exploring its use for conditions like Alzheimer’s Disease, chronic pain, and neurological conditions. TMS’s growing evidence base makes it a respected and trusted treatment option for patients seeking real, measurable relief.
When starting TMS Therapy Near Me, your first step is a consultation with a healthcare professional to evaluate your symptoms, medical history, and treatment goals. If you’re a good candidate, you’ll receive a personalized treatment plan, typically involving 5 sessions per week for 4 to 6 weeks. Each TMS session lasts about 19 minutes and is conducted in a comfortable outpatient setting. There’s no anesthesia, and you can resume normal activities immediately. Many patients begin noticing significant improvements in mood, energy, and focus within a few weeks.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
You can find more information in our Cookie Policy and Privacy Policy.